Intra Uterine Insemination - IUI
What is IUI?
IUI (Intrauterine Insemination) is a simple fertility treatment that helps increase the chances of pregnancy by placing healthy, specially prepared sperm directly inside the uterus at the time of ovulation (egg release).
Breaking it down:
Intra – inside
Uterine – the uterus
Insemination – placing sperm
In this procedure, sperm is washed, concentrated, and placed beyond the cervix, directly into the uterus. This means the sperm is positioned much closer to the fallopian tubes at the exact time the egg is released, improving the chances of fertilization.
Who Can Benefit from IUI?
Male Factor Infertility
IUI can help when sperm-related issues make natural conception difficult, such as:
Oligospermia – low sperm count
Asthenospermia – poor sperm motility (slow-moving sperm)
Teratospermia – high percentage of abnormally shaped sperm
Hypospermia – low semen volume
Viscous semen – overly thick or sticky semen
Use of frozen semen samples
Anatomical defects in the male reproductive tract
Retrograde ejaculation (when semen enters the bladder instead of exiting normally)
Azoospermia with donor sperm
Problems in sexual relations or performance difficulties during timed intercourse
Absentee husband (due to job or travel)
Female Factor Infertility
IUI can also help women with conditions that make natural conception harder, such as:
Poor or hostile cervical mucus
Abnormal Post-Coital Test (PCT) results
Immunological factors at the cervix
Anatomical problems with the uterus or cervix
Poor or irregular ovulation
Unexplained Infertility
In many couples, no specific cause of infertility is found. IUI is often recommended as an initial treatment to improve the chances of pregnancy in such cases.
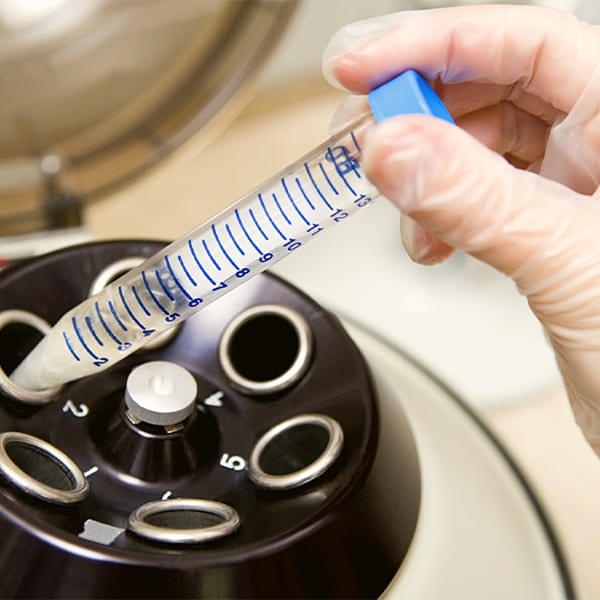
How is IUI treatment done?

For the Female Partner
Ovulation Induction – Medications (tablets or injections) are given to stimulate the ovaries so that multiple eggs are available at the right time.
Monitoring – Follicle growth is tracked using Transvaginal Sonography (TVS).
Ovulation Trigger – When follicles are mature, an hCG injection is given to complete egg maturation and trigger release.
Sperm Placement – A prepared sperm sample (washed semen) is placed directly into the uterus using a thin, soft tube (cannula). The procedure takes only a few seconds and is painless.
Post-Procedure Care – The woman rests for about 10 minutes and can then return to normal activities, including office work, travel, or household tasks. There are no restrictions on intercourse after IUI.
For the Male Partner
Semen Collection – The semen sample is collected on the day of IUI, usually 1–2 hours before the procedure. It can also be collected earlier and stored.
Collection Options – Semen may be collected at the hospital or at home (safely transported).
Frozen Semen – If the husband is unavailable or unable to provide a sample, frozen semen can be used. Men undergoing medical treatments that may affect fertility can freeze semen for future use.
Cryoaccumulation – Multiple semen samples can be frozen and combined for insemination when sperm count is low.
Laboratory Procedure – Sperm Preparation (Semen Wash)
Raw semen contains not only sperm but also other unwanted substances. In our advanced laboratory:
Only the best motile and healthy sperm are separated.
Unwanted material is removed.
Sperm are “capacitated,” a process that makes them ready for fertilization.
Depending on the semen quality, our team chooses the most suitable sperm preparation method to ensure the best outcome.
Insemination Procedure
The insemination itself is a very simple and safe procedure:
The patient is taken to the procedure room/OT.
A comfortable position is given.
Aseptic precautions are followed to maintain hygiene.
A speculum is inserted to visualize the cervix.
The cervix is gently cleaned.
A thin, soft cannula is passed into the uterus.
The prepared sperm sample is slowly injected into the uterus.
The process is quick, painless, and does not require anesthesia.
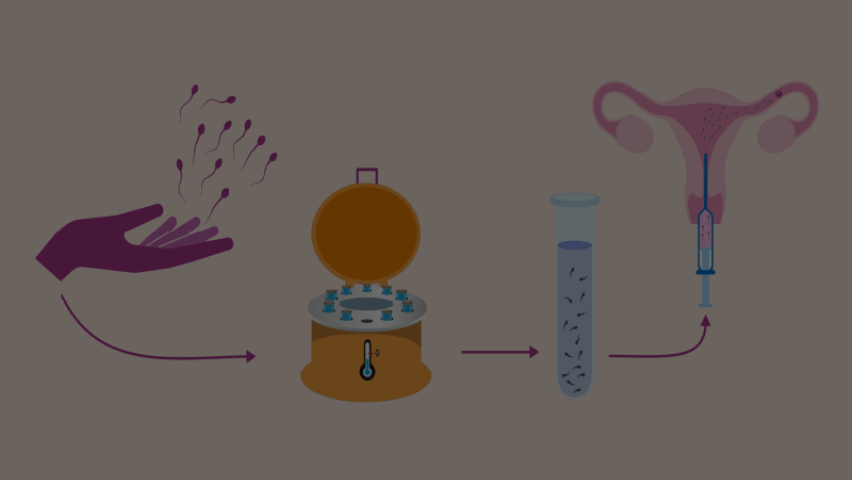
What Medications Are Used During IUI?
Medications play an important role in improving the success of IUI (Intrauterine Insemination). They help stimulate the ovaries, trigger ovulation, and support the uterus for implantation.
1. Ovulation Induction Medications
These medicines are used to stimulate the ovaries to produce one or more mature eggs:
Clomiphene Citrate (Clomid): Often the first-line treatment to induce ovulation.
Letrozole (Femara): Another commonly used oral medication, especially effective in certain patients like those with PCOS.
Gonadotropins (FSH & LH Injections): Injectable hormones that directly stimulate the ovaries for follicle (egg) growth.
2. hCG (Human Chorionic Gonadotropin) Trigger
Once the eggs are mature, an hCG injection is given. This acts as a “trigger shot” to induce final egg maturation and ensure timely ovulation.
3. Progesterone Supplements
After the IUI procedure, progesterone may be prescribed in the form of oral tablets, injections, or vaginal capsules. This helps support the uterine lining and increases the chances of successful implantation and pregnancy.
How Effective is IUI in Achieving Pregnancy?
Intrauterine Insemination (IUI) is a widely used fertility treatment in which prepared sperm is placed directly into the uterus to increase the chances of pregnancy.
On average, IUI has a success rate of about 10–20% per cycle. The success of IUI depends on several factors:
Age: Younger women generally have higher chances of conception.
Fertility Issues: IUI is most effective for couples with unexplained infertility or mild male factor infertility.
Ovulation Induction: Using medications to stimulate ovulation increases the number of available eggs, improving success rates.
Sperm Quality: Higher motility and healthier sperm improve the chances of fertilization.
Lifestyle & Health: Overall health, nutrition, and lifestyle choices can influence outcomes.
Many couples may require multiple IUI cycles to achieve pregnancy. With careful evaluation, proper timing, and advanced laboratory techniques, IUI can be a safe, simple, and effective first step toward starting a family.
Advantages of IUI
Simple and quick procedure: IUI is minimally invasive and painless.
Cost-effective: It is less expensive compared to advanced fertility treatments like IVF.
Improved chances of pregnancy: IUI increases the likelihood of conception compared with natural intercourse, especially in mild infertility cases.
Limitations / Disadvantages of IUI
Requires healthy sperm: Millions of motile sperm are needed for the procedure to be effective.
Fertilization is not guaranteed: We cannot directly observe fertilization or embryo development.
Embryo implantation not assured: Placement in the uterus does not guarantee that an embryo will implant.
Lower success compared to IVF: Success rates are generally lower than advanced ART procedures.
Rare risks: There is a small chance of infection or minor bleeding.
